Number of PAs Continued to Grow for the Past 4 Years Triggering a Vicious Cycle: Reduced Employment Opportunities for Specialists Discourages Residents from Applying
“Our main tasks are notifying the patient’s condition, making rounds, and discussing surgery with the patients: things that residents should do. The PAs mostly write the prescriptions, including those for antibiotics. How is that possible? Professors give us their IDs, so we can take care of the tasks. We do the work because our boss tells us to, but I often feel guilty because I feel like I’m depriving a patient of the right to consult a doctor.”
This is the confession of a nurse (A) who has worked for five years. A introduced herself as a physician assistant (PA), who worked in one of the “big 5” hospitals. After introducing herself, the first words A spoke were that she felt guilty each time she looked after the patients.
A said, “Each time I have patients come to me to receive treatment and prescriptions, when they should be treated by a doctor, I feel guilty because of the thought that I am depriving them of their right to duly consult a doctor.”
A bigger problem is that A is carrying out such tasks without adequate training. A said, “The PAs perform the residents’ tasks without proper education or qualifications. We often work with the residents from other departments, and sometimes there are communication issues between the residents and the nurses.” A complained, “I started working as a nurse because looking after sick people was rewarding, but I can no longer make myself happy.”
Number of PAs in National Hospitals More than Doubled in the Past 4 Years
The biggest problem with the PA system is that eventually it is harmful to the people’s health. If all kinds of illegal medical practices by PAs prevail, such as carrying out operations and procedures or writing prescriptions, which should be done by a doctor, then eventually the people are bound to suffer.
Every year, a stream of accidents occurs due to illegal prescriptions written by people not qualified, just as A confessed. In addition, if the patient’s condition deteriorates, it is unclear as to who should be responsible. According to civil, criminal and administrative law, the PA has no right to hold the person with the doctor’s license responsible.
That’s not all. The PA, who conducted the treatments and provided prescriptions without a doctor’s license, also becomes a criminal who apparently violated the Medical Service Act.
The PA system also has a negative impact on fostering specialists.
Surgery departments, which lack resident applicants, tend to have many PAs. Hospitals illegally delegating medical practices such as surgeries and prescriptions to them eventually deprive residents of a training opportunity.
This can also trigger a vicious cycle, in which the reduced employment opportunities for specialists discourage doctors from applying for resident positions in surgery departments.
However, the number of PAs continues to grow every year.
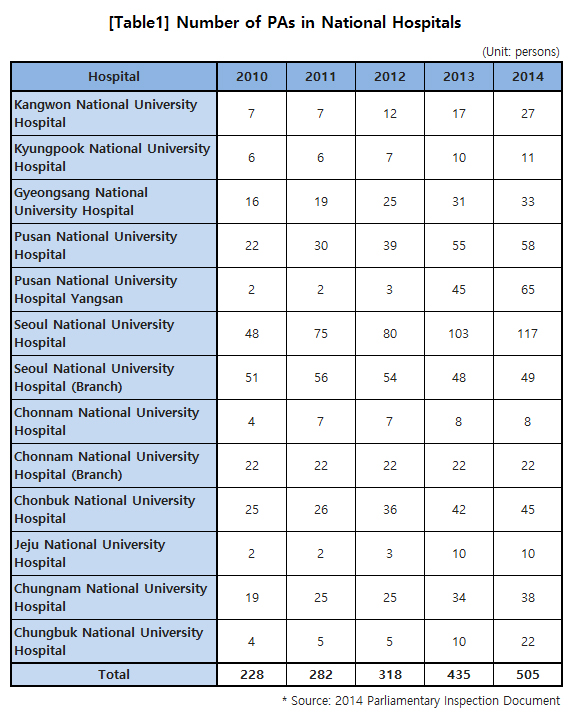
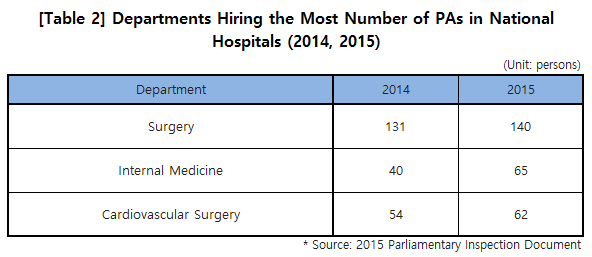
According to the data from a parliamentary inspection in 2014, the number of PAs in national hospitals more than doubled from 228 in 2010 to 505 in 2014. The departments that have a large number of PAs are surgery, followed by internal medicine and cardiovascular surgery. Of the 505 PAs in 2014, 225 (44.5%) worked in one of these three departments.
Residents in these departments traditionally suffer from a heavy task load, so they tend to use more PAs than other departments. In the 2015 parliamentary inspection, lawmakers also pointed to the fact that the number of PAs in national hospitals increased by more than 10% compared to the previous year and suggested that their number be reduced to a minimum, due to potential legal problems when PA-related medical accidents occur. However, government measures to improve the situation remain insufficient.
Chairman Gi Dong-hun, “We Should Call Them UAs not PAs.”
Gi Dong-hun , chairman of the Korean Intern Resident Association, also spoke on the PA system and said, “First, PAs should be called UAs, short for unlicensed assistants. When the working hours of residents were reduced due to a special bill concerning residents, some hospitals hired UAs instead of doctors, such as hospitalists, to fill their hours, and committed a crime by making them examine the patients, write prescriptions, and make rounds.”
He added, “Since the hospitals do not notify the patients that they are being treated by a UA instead of a doctor, patients naturally think that the person treating them is a doctor. But this deprives the patient of his right to consult a doctor and can endanger the patient, for an immediate response may be difficult in an emergency.”
Gi argued that the reason the PA system is now so rampant is because South Korea leaned on expedient measures to solve the problem of medical personnel. Gi said, “If we cannot hire doctors with the current (health insurance) fee, then we should pressure the government to raise the fee. And if the hospital doesn’t have enough doctors, they should reduce the number of patients and delay the surgery. The complaints and damages suffered by the patients because of this is solely the government’s fault, but why should hospitals resort to expedient measures to solve this problem, hiring nurses and making them treat the patients. It is frustrating that the patients, hospitals, doctors and UAs are being held responsible.

