The National Health Insurance Service’s drug price assessment committee recently evaluated Takeda’s Alunbrig (ingredient: briganitib) as eligible for insurance benefit.
The medicine is a second-line treatment for anaplastic lymphoma kinase (ALK)-positive advanced non-small cell lung cancer (NSCLC), approved in Korea late last year.
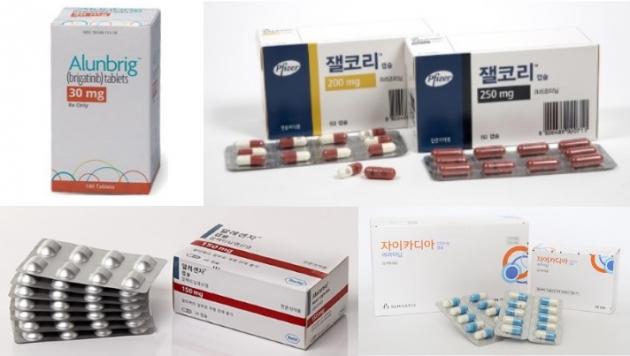
If Takeda successfully proceeds with a drug pricing negotiation with the government, rival drugs such as Pfizer’s Xalkori (crizotinib), Novartis’ Zykadia (ceritinib), and Roche’s Alecensa (alectinib) will face different situations depending on their market share, industry watchers said.
The NHIS’ drug assessment committee on Thursday decided that Alunbrig could become reimbursable for ALK-positive NSCLC.
Observers said Takeda’s obtaining the committee’s reimbursement decision for Alunbrig was incredibly fast. If the company reaches a drug price agreement smoothly within 60 days, Alunbrig will get insurance coverage in April or May, they said.
With a positive outlook for Alunbrig’s reimbursement, rival drugs could fare better or worse, depending on their market status.
Pfizer’s Xalkori, which has been leading the first-line treatment market for ALK-positive NSCLC, could maintain its strength.
However, Novartis’ Zykadia and Roche’s Alecensa might lose out in both first-line and second-line treatment market.
Xalkori has long dominated the targeted therapy market for ALK-positive NSCLC. However, the treatment raised the number of patients with genetic mutation-induced drug resistance. Moreover, the demand for better central nervous system’s response rose, as lung cancer was highly likely to cause brain metastases. Trying to meet the needs, pharmaceutical firms have concentrated on developing improved medicines.
Novartis developed Zykadia and Roche, Alecensa, to shape the second-line treatment market for patients who failed in the first-line Xalkori treatment. The two new drugs extended progression-free survival (PFS) by seven to nine months. With improved efficacy and safety, Zykadia and Roche quickly joined the first-line treatment market.
In Korea, Xalkori, Zykadia, and Alecensa are reimbursable as the first-line treatment for ALK-positive NSCLC, and Zykadia and Alecensa, as the second-line one.
Zykadia and Alecensa, which obtained insurance coverage for the first-line treatment in late 2018, have limited access to clinical use because there is no follow-up drug in case the two drugs fail in the first-line therapy.
Takeda’s Alunbrig arrived in Korea in late 2018, too. The new treatment sold rapidly for patients who failed in the Xalkori therapy, much faster than other ALK inhibitors.
Among patients who failed the Xalkori treatment, Zykadia’s progression-free survival marked 7.2 months, Alecensa, 8.9 months, and Alunbrig, 16.7 months, in the second-line treatment. The central nervous system’s response rate stood at 36 percent in Zykadia, 57 percent in Alecensa, and 67 percent in Alunbrig.
If Alunbrig receives insurance benefit for the second-line treatment, it will come with the condition, “in patients who failed the Xalkori treatment.”
Patients will have to give up a second-line treatment and use a better drug than Xalkori at the time of the first-line treatment or use more potent Alunbrig after Xalkori treatment. They will have to consider the extension of survival time and treatment cost at the same time.
If Alunbrig gets reimbursement as the second-line treatment, Xalkori will be able to maintain its lead in the first-line treatment for a short period because Takeda is expected to challenge the first-line treatment market with Alunbrig shortly, industry watchers said.
In contrast, Zykadia and Alecensa are expected to face difficulties in both first-line and second-line therapy market because Alunbrig is soon to arrive in the first-line market.
“Alunbrig had about twice the progression-free survival compared to conventional treatment in patients with ALK-positive NSCLC who were previously treated with crizotinib. It also showed a wide coverage for genetic mutations and user convenience of a once-daily dose of one tablet,” an official at Takeda said, showing confidence before the market release of the drug.

