Korean researchers have found a new method to quickly heal the wounds of patients with chronic inflammation who are suffering from autoimmune diseases such as rheumatism.
Park Sung-ho, a professor at the School of Life Science of Ulsan National Institute of Science and Technology (UNIST), said Tuesday that he had found that a protein called “SREBP2” regulates the role of macrophages in the inflammatory response, through a joint research with a team at Hospital for Special Surgery, a U.S. hospital specializing in orthopedics,
SREBP2 has been known as a substance controlling cellular cholesterol metabolism.
Wounds heal as inflammatory cells catch harmful bacteria and regenerate the damaged area. The immune cells that are active at this time are macrophages. However, the regeneration of the skin by macrophages does not work properly in patients with chronic inflammation.
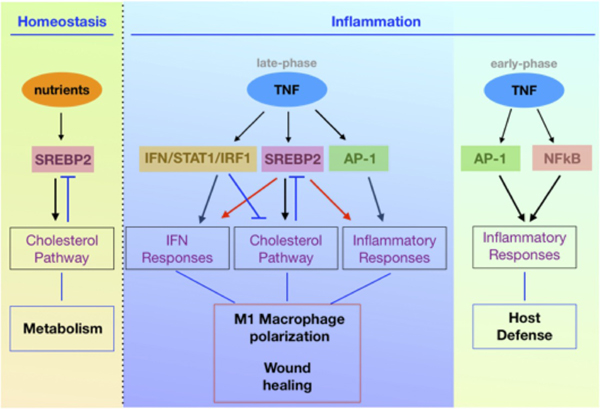
In the early stage of the wound’s healing, macrophages kill harmful bacteria by causing inflammatory responses. In the later stage, they help regenerate the skin around the wound. During this process, tumor necrosis factor (TNF), an inflammatory mediator that calls on macrophages and various inflammatory cells, is used.
However, studies on the TNF-induced macrophage activation response had focused mainly on the early stages of inflammation, and the late-phase regeneration mechanism had remained unclear, the researchers said.

The research team, however, discovered that TNF caused SREBP2 to increase towards the late-phase inflammation and regeneration of the wound.
The researchers also found that SREBP2 binds to inflammatory genes, causes macrophages to make inflammatory responses, and slows the wound repair.
They injured SREBP2 production-inhibited rats and the control mice, and found that injury recovered more rapidly in the former group.
“The study identified SREBP2’s new function and the mechanism of wound healing. It is meaningful that we found a new target substance to develop a treatment to heal wounds of patients with autoimmune diseases,” Park said.
Supported by the U.S. National Institute of Health and the Scleroderma Foundation, the study was published in the journal Immunity on Aug. 20.

