New research shows nine out of 10 young adults in Korea do not have antibodies that protect against hepatitis A, pointing out a need for additional “catch-up” vaccination programs for the most vulnerable.
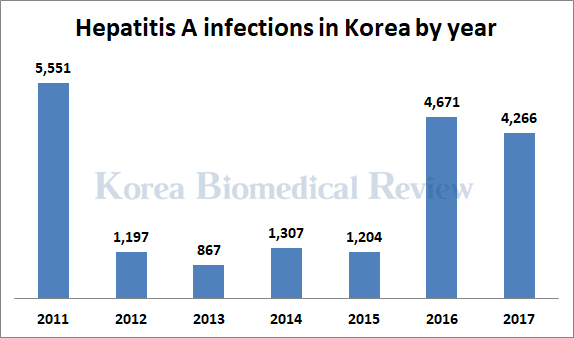
Hepatitis A is an acute inflammatory liver disease caused by the hepatitis A virus (HAV). The condition is highly contagious and often spreads quickly through work and school communities. The rate of hepatitis A infections in Korea has been rising for the second consecutive year, according to the Korea Centers for Disease Control and Prevention.
Researchers from Seoul National University Hospital uncovered the effectiveness of the national childhood hepatitis A vaccination program by looking at the presence of anti-HAV antibodies in 5,856 people over 10 years of age who responded to a government survey in 2015.
The study showed 72.5 percent Koreans in 2015 had anti-HAV antibodies, meaning that they were immune to hepatitis A.
By age bracket, those older than 45 years old had the highest resistance with 97.8 percent of the demographic having anti-HAV antibodies, followed by the 30- to 44-year-olds (90 percent), and 10- to 14-year-olds (59.7 percent)
Only 11.9 percent of those 20 to 29 years of age and 24 percent of those 15 to 19 years old had anti-HAV antibodies, creating a U-shaped curve with the youngest and oldest age brackets having higher resistance to the infection.
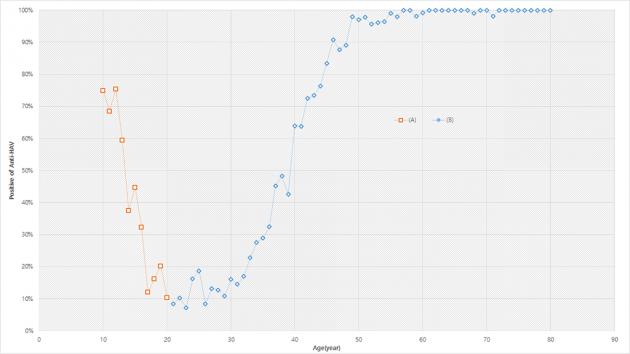
The reason for the U-shaped curve may be a shift from natural infection-induced resistance to vaccine-induced resistance due to rising public health in the nation, coupled with government policy, the study said.
Older Koreans gained immunity mostly through natural infection while the youngest generation gained it through HAV vaccines. But because HAV vaccines were not widely used before the 2000s, those in their 20s remain the most exposed, it noted.
The government had included the hepatitis A vaccine in the national childhood vaccine program since 1997 but left the cost uncovered, leading to a lower vaccination rate among those from low-income families.
“Since HAV vaccination from the National Childhood Vaccine Program in 1997 was a matter of choice, factors such as income and health awareness contributed to differences in anti-HAV positivity,” the study said.
The government-funded nationwide routine vaccination program for children younger than 12 years started much later in 2015.
Non-vaccinated adolescents and young adults should check for hepatitis A antibodies during health checkups and get the vaccine, the researchers emphasized. HAV vaccines are highly effective in preventing hepatitis A in individuals by reducing incidence by more than 90 percent and costs around 70,000 to 80,000 won.
The study also suggested creating additional vaccination programs to protect the exposed age groups.
“We suggest that catch-up HAV vaccination directed at individuals aged 10 to 49 years (or at least among children) should be considered, in addition to the current vaccination program,” the researchers said. “This strategy would rapidly reduce the disease burden of hepatitis A not only in South Korea and but also in other countries which are experiencing a similar epidemiologic shift to Korea.”
The findings were published in the international journal PLOS ONE.

