Doctors criticize law allowing self-determination for ‘not reflecting reality’
After much difficulty, the government has enacted a law that gives patients the right to “die well.” The new law, however, is caught in a controversy over encouraging the meaningless extension of patients’ life. The medical community, while pointing out the law does not reflect the reality at all, is calling for its revision even before its implementation.
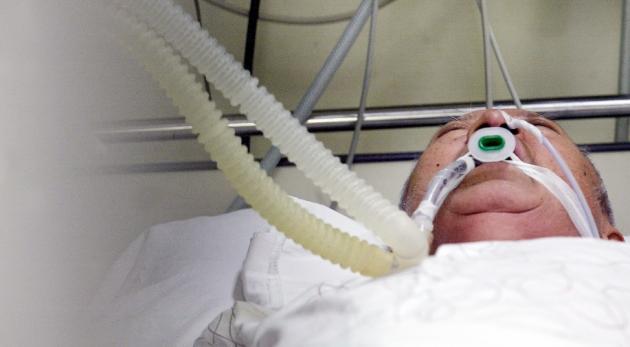
The “act on determining medical care to prolong life,” or more formally the Law to Give Self-determining Right to Continue Medical Treatment to Patients in Hospice, Palliative Care or Dying Process, has allowed terminally-ill patients to decide on their own to stop receiving treatment. Medical care for life prolongation means various treatments, such as the respirator, Cardio Pulmonary Resuscitation (CPR), hemodialysis, and anticancer therapy, to extend patients’ lives with no therapeutic effects. Some parts of the law, such as those concerning hospice and palliative care, will go into effect in August, and those on decision-making to prolong life, from next February.
Under the law, patients will express their intention to discontinue treatments to prolong life in principle. If patients did not make an “advance directive” or cannot make clear their intentions, two or more people from among their spouses, parents or children, have to agree on stopping life-sustaining treatment. If patients had expressed their intentions, their doctors and one medical specialist have to agree that “the deaths are imminent with no chances of recovery” to stop life-sustaining medical care.
The medical community, however, is opposing the law, saying it is unrealistic. For example, critics point to the provision of the law, which calls for asking for the intentions of patients and tape-recording their answers when the patients are too feeble to sign their directives.
Another problem is the provision that excludes medical residents from doctors qualified to judge on the possibility of recovery as well as the designation of relatives and agents. Seniors without families or those with families who refuse to discuss the patients’ life or death need agents but the law does not allow for this, the critics say. Also problematic are undue documentation and excessive rules of punishment, the opponents say.
“The authors of the law say it applies only on special situations in which decision to discontinue medical care can be a problem, but there are no definitions about such special circumstances in both the law and lower statutes,” said Professor Choi Hae-jin at Yonsei University College of Medicine. “As it is difficult to define the particular situation from clinical aspects, the law is highly likely to be applied to all dying patients contrary to its original intention.”
“Do you think it possible at all we can make dying patients agree to stop medical care or tape-record their words in a critical situation,” she said. Medical will have no choices but to continue to provide medical care if for no other reason that being embroiled in medical lawsuits.”
Thirteen academic organizations, including Korea Cancer Association and the Korean Society for Medical Ethics, called for the government to start with pilot projects before implementing the law, pointing out these and other problems.
“The law is designed to help terminally-ill patients to die a comfortable death but can end up only extending meaningless medical treatment,” they said in a statement issued on April 26. “The expressions and standards in the law are vague, causing serious confusion in its interpretation. To prevent the chaos, the government should start with a pilot project before it takes root while shelving its punishing rules.
The government says it would correct some problems through lower statutes. “The medical community is pointing to the excessive documentation, but the government has just made standard forms, as the law calls for offering the legal basis for continuing or stopping medical care to prolong lives,” said Hwang Eu-soo, director of the Life Ethics Policy Division at the Ministry of Health and Welfare. “The recording is just a complimentary method. We will reflect opinions from the medical field on the law.”

